Dinamika okužb s Covid-19 v Indiji je v spodnji sliki. Vsi smo gledali grozljive prizore iz Indije spomladi letos. Bolnišnice so bile prepolne, ljudje so umirali na ulicah. Vsi so pričakovali, da se bo število okužb še bolj povečalo. Pa je nenadoma upadlo. Z enakim eksponentnim trendom, kot je malce prej naraščalo. In nihče ne ve, zakaj. Zaradi vroče in vlažne klime? Zaradi nošenja mask? Zaradi slabega zdravstva in posledično boljšega imunsklega sistema zaradi predhodno prebolelih bolezni od malarije naprej? Zaradi mlade demografije? Za vsako izmed teh teorij obstaja nasprotna, ki kaže, da bi lahko bilo diametralno nasprotno.
V resnici na ljubo znanost glede tega povsem tava v temi. Spodaj je najboljši posnetek možnih razlag, ki sem ga našel (kliknite na povezave). Vendar pazite: te razlage se nanašajo na indijski prvi val, ki je dosegel vrh lani sredi septembra in se izpel. Nakar se je konec februarja začel drugi val, bistveno bolj drastičen, dosegel vrh v začetku maja. In uplahnil. In tako kot po prvem valu, tudi po drugem znanstveniki tavajo v temi in iščejo možne razlaga. No, hipoteze. Za nobeno izmed njih (še) ni potrditve.
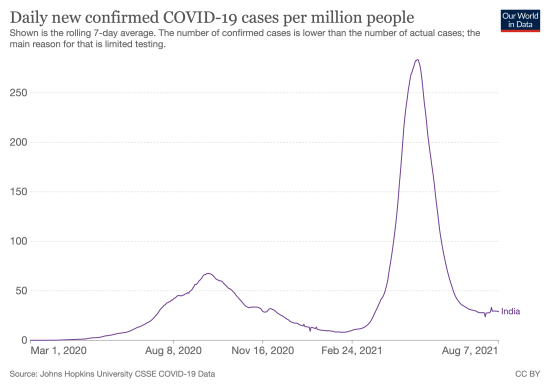
India’s climate and demographics have not changed during the pandemic. And the drop in India’s COVID-19 caseload has been recent. It hit a peak in September and has declined inexplicably since then.
In fact, India’s numbers went down exactly when experts predicted they would spike: in October, when millions of people gathered for the Hindu festivals of Diwali and Durga Puja. It’s when air pollution is also worst, and experts feared that would exacerbate the pandemic too.
Cases have also declined despite what many thought would be a superspreader event: tens of thousands of Indian farmers camping out on the capital’s outskirts for months.
“Three options: One is that it’s gone because of the way people behaved, so we need to continue that behavior. Or it’s gone because it’s gone and it’s never going to come back — great!” says Das, from Georgetown. “Or it’s gone, but we don’t know why it’s gone — and it may come back.”
…
“It’s the million-dollar question. Obviously, the classic public health measures are working: Testing has increased, people are going to hospitals earlier and deaths have dropped,” says Genevie Fernandes, a public health researcher with the Global Health Governance Programme at the University of Edinburgh. “But it’s really still a mystery. It’s very easy to get complacent, especially because many parts of the world are going through second and third waves. We need to be on our guard.”
Scholars are examining India’s mask mandates and public compliance, as well as its climate, its demographics and patterns of diseases that typically circulate in the country.
…
Aside from mask compliance, there’s also India’s climate: Most of the country is hot and humid. That too has deepened the mystery. There’s some evidence that India’s climate may help reduce the spread of respiratory viruses. But there’s also some evidence to the contrary.
A review of hundreds of scientific articles, published in September in the journal PLOS One, found that warm and wet climates seem to reduce the spread of COVID-19. Heat and humidity combine to render coronaviruses less active — though the certainty of that conclusion, the review says, is low. Previous research has also found that droplets of the virus may stay afloat longer in air that’s cold and dry.
…
But there’s also some scientific evidence to the contrary, that India might actually be more conducive to the coronavirus: Research published in December in the journal GeoHealth says that urban India’s severe air pollution might exacerbate COVID-19. Not only does pollution weaken the body’s immune system, but when air is thick with pollutants, those particles may help buoy the virus, allowing it to stay airborne longer.
A paper published in July in The Lancet says extreme heat may also force people indoors, into air-conditioned spaces — and thus might contribute to the virus’s spread. The Natural Resources Defense Council has warned that extreme heat can lead to a spike in other illnesses — dehydration, diarrhea — that might lead to overcrowding in hospitals and clinics already struggling to treat victims of COVID-19.
…
Another point to consider about India is how many other diseases are already rampant: malaria, dengue fever, typhoid, hepatitis, cholera. Millions of Indians also lack access to clean drinking water, sanitation and hygienic food. Some experts speculate that people with robust immune systems may be more likely to survive in India in the first place.
“All of us have pretty good immunity! Look at the average Indian: He or she has probably had malaria at some point in his life or typhoid or dengue,” says Sayli Udas-Mankikar, an urban policy expert at the Observer Research Foundation in Mumbai. “You end up with basic immunity toward grave diseases.”
Two new scientific papers support that thesis, though they have yet to be peer-reviewed: One study by Indian scientists from Chennai and Pune, published in October, found that low- and lower-middle-income countries with less access to health care facilities, hygiene and sanitation actually have lower numbers of COVID-19 deaths per capita. Another study by scientists at India’s Dr. Rajendra Prasad Government Medical College, published in August, found that COVID-19 deaths per capita are lower in countries where people are exposed to a diverse range of microbes and bacteria.
But experts warn that these two studies are preliminary and should serve only as a springboard for more investigation.
“They’re not based on any biological data. So they’re good for generating a hypothesis, but now we really need to do the studies that will result in explanations,” says Dr. Gagandeep Kang, an infectious diseases researcher at the Christian Medical College in Vellore. “I hope scientists work more on this soon. We need deeper dives into India’s immune responses.”
…
India is a very young country as well. Only 6% of Indians are older than 65. More than half the population is under 25. Those who are young are less likely to die of COVID-19 and are more likely to show no symptoms if infected.
A study of nearly 85,000 coronavirus cases in India, published in November in the journal Science, found that the COVID-19 mortality rate actually decreases there after age 65 — possibly because Indians who live past that age are such outliers. There are so few of them.
Vir: Lauren Frayer, NPR
V Indiji se je umrljivost od Covida 19 občutno zmanjšala od trenutka, ko so prenehali upoštevati navodila WHO in so pričeli uporabljati zdravilo ivermectin. Indijska zastopnica WHO dr. Soumya Swaminathan se je seveda temu upirala, sedaj pa jo tožijo zaradi odgovornosti za smrt več tisoč Indijcev in ji grozi kazen s smrtjo ali dosmrtna ječa.
Všeč mi jeVšeč mi je
Točno tako. S tem, da niso vse indijske države začele uporabljati ivermectina glej:
“Cases in Delhi, where Ivermectin was begun on April 20, dropped from 28,395 to just 2,260 on May 22. This represents an astounding 92% drop. Likewise, cases in Uttar Pradesh have dropped from 37,944 on April 24 to 5,964 on May 22 – a decline of 84%.”
“Meanwhile, Tamil Nadu announced on May 14 they were outlawing Ivermectin in favor of the politically correct Remdesivir. As a result, Tamil Nadu’s cases are up in the same time frame from April 20 to May 22 – 10,986 to 35,873 – more than a tripling.”
A li se vam ne zdi čudno, da tega dejstva “čuveni” Lancet ne omenja. Nekako ne gre v zgodbo o cepivih kot edini zanesljivi obrambi proti Covid-19
Všeč mi jeVšeč mi je
Kaj pa Peru?
https://healthfeedback.org/claimreview/no-data-available-to-suggest-a-link-between-indias-reduction-of-covid-19-cases-and-the-use-of-ivermectin-jim-hoft-gateway-pundit/
Všeč mi jeVšeč mi je
Ah, še nekaj sem pozabil. WHO namreč.
Vse kar počne in priporoča WHO je potrebno jemati z rezervo. Države namreč pokrivajo samo eno petino proračuna, 4/5 pa privatni donorji, predvsem farmacevtska industrija. Med njimi je največji Bill& Melinda Gates Foundation, ki direktno in preko GAVI (Global Alliance for Vaccine Initiative), ki ga kontrolira, prispeva letno približno 430 milijonov USD. To je mislim več kot katerakoli država.
Mimogrede Bill Gates je direktno in indirektno tudi največji posamezni investitor (več mrd USD) v BioNtech in Moderno tj. izdelovalca mRNA cepiv proti Covid-19. Gre za masovni konflikt interesov o katerih naši in tuji novinarji, sami Sherlock Holmes-i, ne črhnejo niti besede….In kljub temu, da je delež smrti na 100.000 cepljenih pri mRNA cepivih 3 do 5x večji kot pri vektorskih, slišite samo o komplikacijah z vektorskimi cepivi.
https://www.rt.com/russia/522084-hungary-vaccination-stats-sputnik/
Ali ni to čudno?
Nisem strokovnjak za viruse in cepiva, ampak na denar se kot dolgoletni finančni direktor malce spoznam. In na vpliv, ki ga ima na ljudi. In nekaj vam povem:
ljudje praviloma delajo za tistega, ki jih plačuje.
Všeč mi jeVšeč mi je
G. Golob, se strinjam z vsem napisanim in upam, da ne boste prenehali z objavljanjem resnice, kajti le-ta je danes v hudem pomanjkanju. Žal se teorije zarote danes uresničujejo ena za drugo in kdor tega še ni spoznal, je kot tisti noj, ki tišči glavo v pesek. Vedno hitreje drsimo v totalno diktaturo, v kateri ljudje ne bomo brez dovoljenja zdravniško-politične mafije smeli niti ven iz stanovanja. Kot primer totalne norosti lahko pogledamo petmiljonski Sidney, kjer so zaradi dveh smrti od Covida ponovno uvedli lockdown, povišali kazen za nenošenje maske na 500 $ in spodbujajo ljudi na prijavljanje sosedov, ki se ne držijo ukrepov.
https://www.armstrongeconomics.com/international-news/australia-oceania/australia-lockdown-sending-in-military-increase-police-powers-without-limitation/
Gates je seveda na čelu vsega dogajanja, v MSM pa ne zvemo nič, kar ni uradno dovoljeno. Predlagam vsakodnevno branje bloga g. Martina Armstronga, ki je eden od najbolj informiranih ljudi na tem svetu in se ne boji povedati resnice.
https://www.armstrongeconomics.com/international-news/vaccine/covid-pandemic-can-never-end-because-50-of-people-have-been-vaccinated/
Všeč mi jeVšeč mi je
Ste se pa našli teoretiki zarot in antivakserji na tem forumu. Puščam diskusijo, ker je to temelj, da se pride do resnice. Vendar ne pozabite dvojega:
1. relevantna je diskusija na znanstveni ravni (na podlagi kotroliranih eksperimentov, kliničnih testov in empiričnih šudij), ne pa facebook-informirana diskusija ali nizanje anekdotskih argumentov, ki gredo v prid, vendar so anekdotični primeri in ne splošno veljavni pojavi,
2. zmaga tista hipoteza in postane teorija, ki preživi vse preverbe in diskusije. Kar pa je zelo ex post. Torej bo treba počakati na konec epidemije.
Všeč mi jeVšeč mi je